An alternative hip prosthesis called a "cementless" total hip replacement has the potential to allow bone to grow into it, and therefore may last longer than the cemented hip. This is an important consideration for the younger patient. In some cases, only one of the two components (socket or stem) may be fixed with cement and the other is cementless and would be called a "hybrid" hip prosthesis.
When is total hip replacement considered?
Total hip replacements are usually performed for severe arthritic conditions. The operation is sometimes performed for other problems such as hip fractures or avascular necrosis (a condition in which the bone of the hip ball dies). Most patients who have artificial hips are over 55 years of age, but the operation is occasionally performed on younger persons.
Circumstances vary, but generally, patients are considered for total hip replacements if :
- Your pain is severe enough to restrict work, recreation, and the ordinary activities of daily living.
- Your pain is not relieved by anti-inflammatory medicine, the use of a cane or walker and restricting activities.
- You have significant stiffness of the hip.
- Your x-rays show advanced arthritis, or other problems.
What can I expect of a total hip replacement?
A total hip replacement will provide pain relief in 90 to 95 percent of patients. It will allow patients to carry out many normal activities of daily living. The artificial hip may allow you to return to active sports or heavy labor under your physician's instructions. Most patients with stiff hips before surgery will regain near-normal motion, and nearly all have improved motion.
Uncemented / Cementless Total Hip Replacement
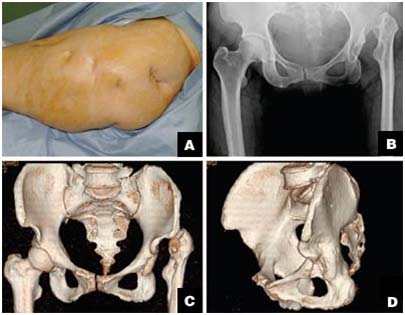 Figure 1 :
Figure 1 : Photograph of the left hip of a 45-year-old woman who suffered infective hip arthritis when she was 3 years old. The photograph shows a previous arthrotomy scar and old draining-sinus scars (A). Radiograph (B) and three-dimensional computed tomographic images (C, D) showing complete resorption of the femoral head, a high-riding hip center, a dysplastic acetabulum with deficient bone stock, and a hypoplastic femur with a small canal diameter.
In the 1980s, new implant designs were introduced to attach directly to bone without the use of cement. In general, these designs are larger and longer than those used with cement.
They also have a surface topography that is conducive to attracting new bone growth. Most are textured or have a surface coating around much of the implant so that the new bone actually grows into the surface of the implant. Because they depend on new bone growth for stability, cementless implants require a longer healing time than cemented replacements.
The orthopaedic surgeon must be very precise in preparing the femur for a cementless impact. The implant channel must match the shape of the implant itself very closely. New bone growth cannot bridge gaps larger than 1 mm to 2 mm.
Your surgeon may recommend a period of protected weight-bearing (using crutches or a walker) to give the bone time to attach itself to the implant. This protected weight bearing helps to ensure there is no movement between the implant and bone so a durable connection can be established.
Cementless femoral components tend to be much larger at the top, with more of a wedge shape. This design enables the strong surface (cortex) of the bone and the dense, hard spongy (cancellous) bone just below it to provide support.
The acetabular component of a cementless total hip replacement also has a coated or textured surface to encourage bone growth into the surface. Depending on the design, these components may also use screws through the cup or spikes, pegs, or fins around the rim to help hold the implant in place until the new bone forms. Usually these components have a metal outer shell and a polyethylene liner.
The pelvis is prepared for a cementless acetabular component using a process similar to that used in a cemented total hip replacement procedure. The intimate contact between the component and bone is crucial to permit bone ingrowth.
Initially, it was hoped that cementless total hip replacement would eliminate the problem of bone resorption or stem loosening caused by cement failure. Although certain cementless stem designs have excellent long-term outcomes, cementless stems can loosen if a strong bond between bone and stem is not achieved.
Patients with large cementless stems may also experience a higher incidence of mild thigh pain. Likewise, polyethylene wear, particulate debris, and the resulting osteolysis (dissolution of bone) remain problems in both cemented and uncemented designs. Improvements in the wear characteristics of newer polyethylene and the advent of hard bearings (metal-on-metal or ceramic) may help resolve some of these problems in the future.
Although some orthopaedic surgeons are now using cementless devices for all patients, cementless total hip replacement is most often recommended for younger, more active patients and patients with good bone quality where bone ingrowth into the components can be predictably achieved. Individuals with juvenile inflammatory arthritis may also be candidates, even though the disease may restrict their activities.
What are the risks of total hip replacement?
Total hip replacement is a major operation. The effect of most complications is simply that the patient stays in the hospital longer. The most common complications are not directly related to the hip and do not usually affect the result of the operation. These include :
- Blood clots in the leg
- Urinary infections or difficulty urinating
- Blood clots in the lung
Complications that affect the hip are less common, but in these cases, the operation may not be as successful :
- Difference in leg length
- Stiffness
- Dislocation of hip (ball pops out of socket)
- In the hip
A few of the complications, such as infection or dislocation, may require re-operation. Infected artificial hips sometimes have to be removed, leaving a short (by one to three inches), somewhat weak leg, but one that is usually reasonably comfortable and one on which you can walk with the aid of a cane or crutches.
How long will I be in the hospital after surgery?
The hospital stay usually ranges from three to four days. Patients who live with someone who can assist them, are usually able to go home without much problem. However, patients who live alone are encouraged to find someone who can stay with them when they return home. Patients who do not progress well may require a short stay in a rehabilitation center, where they can receive physical and occupational therapy and instruction in how to care for themselves at independently.
How long will I need crutches or a walker?
Most patients use crutches or a walker for about 4-6 weeks or until instructed otherwise by a physician.
What activities can I do following hip replacement?
It takes about three months for the hip to recover to a point where you are back to full activity. Obviously, some patients recover faster and others more slowly depending upon age, health status, personal motivation, and response to rehabilitation. The purpose of hip replacement surgery is to relieve pain, allowing you to return to a high level of function. This means that most activities are okay once you have completely healed. However, most surgeons recommend that you avoid "impact" type of activities, such as running, aerobics, cutting or pivoting sports, or other activities that place a high degree of stress on the hip. Walking, bicycling, swimming, cross-country skiing, golf, and bowling are often approved.
How successful is total hip replacement surgery?
Results are generally very good; most people are relieved of all their hip and groin pain and the replaced joint will usually last ten years, depending on patient use and activity levels.
The major long-term problem is loosening of the prosthesis. This occurs either because the cement crumbles (as old mortar in brick building) or because the bone melts away (resorbs) from the cement.
Loose, painful artificial hips can usually, but not always, be replaced. The results of a second operation are not as good as the first, and the risks of complications are higher.
Preparing for Surgery
Preparing for a total hip replacement begins several weeks before the actual surgery. Maintaining good physical health before your operation is important and activities that increase upper body strength will improve your ability to use a walker or crutches after the operation.
The physician may order blood tests and urinalysis before surgery to make sure that a urinary tract infection is not present. Urinary tract infections are common, especially in older women, and often go undetected. Your Orthopaedic surgeon may ask you to see a medical doctor, especially if medical problems have been present in the past.
It is important that your teeth be in good condition. An infected tooth or gum may be a possible source of infection for the new hip. In addition, any blisters, cuts, or boils should be reported. If infection is found, surgery is generally delayed until the infection is cleared.
Will I need anything special at home?
You will need a hand rails on the stairway into the house, an elevated toilet seat, and crutches or a walker. Optional things include handrails around the toilet, bath areas, and stairwells. Any scatter rugs should be removed and torn areas in the carpet or tile tacked down to prevent falling. In addition, watch out for small pets that may get underfoot!
When preparing for surgery, you should begin thinking about the recovery period after you leave the hospital. Discharge from the hospital is usually in about three to four days and a patient with a new total hip replacement is strongly encouraged to have someone at home to assist with dressing, getting meals, etc. for the first couple of weeks. If assistance from someone at home is not possible please let the discharge planner know. It may be necessary to think about arranging a short-term stay in a skilled extended care facility, an acute rehab unit, or receive therapy at home with in-home care. To qualify for these options, you must meet certain criteria as directed by Medicare and/or your insurance carrier. If needed, outpatient therapy can be arranged in a facility near your home.
Pre-op Visit
Due to changes in insurance coverage, it is necessary for most patients to visit the hospital before their actual surgery date. This visit usually lasts several hours, so plan to spend most of the day.
The day begins in the clinic, where an interview by the nursing staff concerning past medical history and current medications will be taken, as well as a chest x-ray. You may be instructed to stop taking your anti-inflammatory medications (Ibuprofen, Naprosyn, Relafen, DayPro, Aspirin) one week before surgery. You will be attending a teaching session, which will provide you with information about your surgery. There will also be time for discussion and questions. Bring a written list of past surgeries and of the medications and dosages that you normally take at home.
During your pre-op visit, blood will be drawn and lab tests done to insure that you are in good general health. X-rays are taken if necessary. Chest x-rays and an EKG are obtained if you have not had one taken for six months or if otherwise indicated. After all of these tests and exams are completed, a nurse will talk with you to determine the type of anesthesia that is best suited for you. Before you leave the hospital, make sure your questions are answered.
If at any time you become ill, such as with a cold or flu, you need to call your physician. Remember we want you to be in your best possible health!
Pre-op Exercises
Deep Breathing Exercises: You should exercise your lungs every day before surgery by inhaling deeply through your nose, then slowly exhaling through your mouth. Repeat this three times and then cough two times, every 30 minutes. These exercises are necessary to remove any excess secretions that may settle in your lungs while you are asleep during surgery.
Ankle Pumps: You should pump your ankles back and forth 1000 times every day. This is your best defense against blood clots. Crutches/Walker Please bring crutches or a walker with you to the hospital, so we can make sure that the equipment is in good working order and set at the right height for you.
These exercises will be given to you with detailed instructions during your pre-op visit.
Surgical Checklist
Are there any special instructions I should know about?
A shower, bath, or sponge bath should be taken the evening before and the morning of surgery with the medicated liquid soap that was given to you at the time of your pre-admission testing. Nail polish and make-up should be removed.
Unless instructed otherwise, do not eat or drink anything after midnight!
What should I bring to the hospital?
- Crutches or walker
- Good walking shoes (crepe or rubber soles)
- Pair of shorts or sweatpants and a T-shirt
- Pajamas and robe
- Toothbrush, toothpaste, deodorant and other personal items
- Electric razors only!
What happens after I arrive at the hospital?
You should arrive at the hospital at the instructed time and go to the Surgery Prep area. The nurse will spend a few minutes making sure that you are still in good health and ready for surgery. The nurses will try to give you a good estimation of when you will be going into surgery. However, it is hard to predict how long every surgery is going to take, so expect some waiting time and bring something to help pass the time like a magazine, book or other quiet activity.
You will be taken to a pre-surgical care unit where you will be asked to change into a hospital gown. An intravenous (IV) will be started to administer fluids and medications during and after the surgical procedure. From there, you will be transported to the operating room. Your family and/ or friends may accompany you part of the way and then will be instructed to wait in the Surgery Waiting area. Your doctor will talk to your family after the surgery to report your progress.
How long does the surgery take?
The actual surgical procedure usually takes about 1-3 hours. However, preoperative preparation as well as wake-up time may make your operating room and recovery room stay longer.
What should I expect after surgery?
After surgery, you will be taken to the Recovery Room for approximately 2 hours for observation. Your blood pressure, pulse, respiration, and temperature will be checked frequently. Close attention will be paid to the circulation and sensation in your legs and feet. It is important to tell your nurse if you experience numbness, tingling, or pain in your legs or feet. When you awaken and your condition is stabilized, you will be transferred to your room.
Although circumstances vary from patient to patient, you will probably have some or all of the following after surgery :
- You will find that a large dressing has been applied to the surgical area to maintain cleanliness and absorb any fluid. This dressing will be removed within 24 - 48 hours after surgery.
- An IV, started before surgery, will continue until you are taking adequate amounts of fluid by mouth. When you are taking fluids well, the IV may be changed to a Heparin lock, a small sterile tube that will keep a vein accessible for antibiotics and allow for easier movement. Antibiotics are frequently administered every eight hours, for two to three days, to reduce the risk of infection.
- One side effect of anesthesia is often a difficulty in urinating after surgery. For this reason, a sterile tube called a foley catheter may be inserted into your bladder to insure a passageway for urine. It will be removed 24 hours after surgery.
- You will have on intermittent passive compression (IPC) stocking sleeves that are connected to a machine that circulates air in the plastic and around your legs. These stockings are worn on your legs to prevent blood clots from forming after surgery. You will also be given medications and exercise instructions to help to prevent clots.
- Post-operatively you may have temporary nausea and vomiting due to anesthesia or medications, i.e. (PCA). Medication may be given to minimize this.
- Your diet will progress as your condition permits, starting with ice chips and clear liquids.
- To help prevent complications, such as congestion or pneumonia, deep breathing and coughing exercises are important. After surgery, these exercises are to be done every one or two hours. Inhale deeply through your nose; then slowly exhale through your mouth. Repeat this three times and then cough two times. You will be encouraged to use your inspirex, blowing the ball up the tube by taking deep breaths.
A metal triangle called a trapeze will be placed in the overhead bed frame to assist you in moving around the bed. You are encouraged to move in bed without the trapeze. This will help you prepare for independence at home.
Pain Control
An epidural or a patient controlled analgesia (PCA) is used for the first two to three days after your surgery. When the epidural or PCA is discontinued, your doctor will prescribe pain medication to be taken by mouth. It is important to continue taking them because preventing pain is easier than chasing it. If you continue to experience pain after taking the medication, we encourage you to notify your nurse so alternate methods of pain control can be started.
Some patients experience back discomfort after surgery. This is caused by the general soreness of the hip area and partly by the prolonged lack of movement required before, during, and after surgery. Periodic change of position helps to relieve discomfort and prevents skin breakdown.
There will be some precautions, mostly to prevent dislocation, which is more likely to occur the first six to eight weeks after surgery.
These precautions include :
- Using one pillows between your legs
- Not crossing your legs
- Not bending forward 90 degrees
- Using a high-rise toilet seat
- Do not let your knees and/or toes turn in
Patients are usually given blood thinners to prevent blood clots in the leg following the hip replacement. This continues for about three weeks following surgery.
Exercise Therapy and Rehabilitation Program
When muscles are not used, they become weak and do not perform well in supporting and moving the body. Your leg muscles are probably weak because you haven't used them much due to your hip problems. The surgery can correct the hip problem, but the muscles will remain weak and will only be strengthened through regular exercise. You will be assisted and advised how to do this, but the responsibility for exercising is yours.
Physical therapy is started the day after surgery provided there are no complications. You will walk and be assisted into a chair the first day after surgery. During this time, discomfort may be experienced while walking and exercising. The doctor will order pain medication, as needed.
You will work with a physical therapist twice a day to become independent in walking, going up and down stairs, getting in and out of bed, and doing exercises to improve the range of motion and strength of your hip. Therapists will stop or decrease the amount of time they see you when you reach the treatment goals set for you. These goals will be determined by your physical abilities before surgery.
How well you regain strength and motion is, in part, dependent upon how well you follow your physical therapy. This part of your rehabilitation is something that you must do for yourself, and not something someone else does for you.
You will also work with an Occupational Therapist (OT). OT will focus on helping you gain independence through self-care. The second day after your surgery an OT will set you up with bathing and dressing aids. You will have the opportunity to practice using the assistive equipment to complete your home care. Following your total hip replacement precautions is necessary for at least 12 weeks after your surgery. Understanding how to use the equipment will help you maintains the hip precautions.
It takes about three months for the hip to recover to a point where patients are back to full activities. Obviously, some patients recover faster and others slower. Factors like health status, personal motivation, and response to rehabilitation all affect a person's recovery.
Guidelines at Home
What happens after I go home?
Upon discharge from the hospital, you will have achieved some degree of independence in walking with crutches or a walker climbing a few stairs, and getting into and out of bed and chairs. However, someone is needed at home to assist you for the next two weeks or until your energy level and mobility has improved.
Medication
You may be sent home on prescribed medications to prevent blood clots. Your doctor will determine whether you will take a pill (Coumadin or coated aspirin) or give yourself a shot (Enoxaparin). If an injection is necessary, your doctor will discuss this with you. The nursing staff will teach you or a family member what is necessary to receive this medication.
You will be sent home on prescribed medications to control pain. Plan to take your pain medication 30 minutes before exercises. Remember that preventing pain is easier than chasing it. If pain control continues to be a problem, call your doctor.
Exercises
You will be instructed in a home exercise program designed by your physical therapist. Remember that walking is not a substitute for your exercises. If an exercise is causing long-lasting pain, you should cut back on your exercises. If it continues to cause pain, contact your physical therapist or physician.
Activity
Continue to walk with crutches or a walker as directed by the physician or physical therapist. Your physician will determine how much weight you can place on your operated leg.
Walking is one of the best forms of physical therapy and for muscle strengthening.
Are there certain things I need to avoid after my hip replacement?
Yes, there are a number of things you need to be aware of. Your new hip is designed to eliminate pain and increase function. Certain movements place undue stress on your new hip. For your safety, these should be avoided. This is especially true during the first few months after your surgery.
Here is an outline of the precautions you should follow after surgery.
- Riding in a car is permitted as long as you make frequent stops, at least once per hour, to get out and walk around.
- Always sit in a chair with arms. Avoid sitting on low chairs or sofas. Instead sit in a high chair or place a firm cushion on your furniture. Use the armrests on the chair to assist you getting up.
- Do not cross your legs. Always sit with your legs 3 - 6 inches apart.
- Have a pillow between your legs when turning in bed.
- Avoid low or conventional toilet seats. Use a toilet seat riser for the next 12 weeks to avoid excessive bending of the hips. When using a public restroom, you should use the handicapped facilities to ensure adequate toilet height.
- No tub baths, only showers, until hip precautions are discontinued by your physician.
- Sitting in the bottom of your bathtub is forbidden. Do not sit in a bathtub until your physician approves that activity. You may want to get a shower seat for your tub.
- Do not reach down to put on shoes and socks. You may want to get a long handled shoehorn.
- Avoid stooping, squatting or bending forward excessively for the first 6 weeks. Use a reacher if you need something very low.
- Do not turn your knee, hip, or foot inward when sitting, standing, or lying down.
- Avoid sitting more than 60 minutes at a time.
- All furniture that you sit or lie on must be at least 18 inches off the floor.
- It is recommended that you do not drive until three to four weeks following surgery. When getting into a car, back up to the seat of the car, sit and slide across the seat toward the middle of the car with your knees about 12 inches apart. A plastic bag on the seat will help you safely slide in/out of the car.
- Sexual activity can be resumed per your physician's instructions.
- You can usually return to work within three to six months or as instructed by your doctor.
In addition, when visiting physicians and dentists it is important that you inform them that you have a total joint replacement. You will need antibiotics for certain dental and medical procedures, ask your doctor for a medical alert card, if you don't already have one.
This precaution will be permanent
Your incision
Keep the incision clean and dry. Also, upon returning home, be aware of certain warning signs. If any swelling, increased pain, drainage from the incision site, redness around the incision, or fever is noticed, report this immediately to the doctor. Generally, the staples are removed in 2 weeks.
Prevention of infection
If at any time (even years after the surgery) an infection develops such as strep throat or pneumonia, notify your physician. Antibiotics should be administered promptly to prevent the occasional complication of distant infection localizing in the hip area.
Remember : Your physician, physical therapist, and nurses are striving to make a painless, functional hip possible for you. The real success of your hip replacement, however, depends partly on you - especially how conscientiously you exercise and how diligently you apply follow the hip precautions.





