Cemented fixation relies on a stable interface between the prosthesis and the cement and a solid mechanical bond between the cement and the bone. Today's metal alloy stems rarely break, but they can occasionally loosen. Two processes, one mechanical and one biological, can contribute to loosening.
In the femoral component, cracks (fatigue fractures) in the cement that occur over time can cause the prosthetic stem to loosen and become unstable. This occurs more often with patients who are very active or very heavy. The action of the metal ball against the polyethylene cup of the acetabular component creates polyethylene wear debris. The cement or polyethylene debris particles generated can then trigger a biologic response that further contributes to loosening of the implant and sometime to loss of bone around the implant.
The microscopic debris particles are absorbed by cells around the joint and initiate an inflammatory response from the body, which tries to remove them. This inflammatory response can also cause cells to remove bits of bone around the implant, a condition called osteolysis. As the bone weakens, the instability increases. Bone loss can occur around both the acetabulum and the femur, progressing from the edges of the implant.
Despite these recognized failure mechanisms, the bond between cement and bone is generally very durable and reliable. Cemented total hip replacement is more commonly recommended for older patients, for patients with conditions such as rheumatoid arthritis, and for younger patients with compromised health or poor bone quality and density. These patients are less likely to put stresses on the cement that could lead to fatigue fractures.
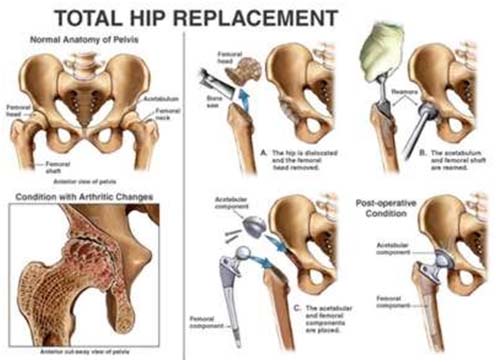 Fig :
Fig : Cemented Total Hip Replacement in India
Cement fixation has a 30-year history in total hip arthroplasty. Cement fixation is a durable and reproducible means of fixation in a variety of hips. A key determinant to a cement mantle’s longevity is the technique of cementing. This article reviews what has been learned in the past and outlines the state of the art in cement technique today.
One of the relatively recent changes in cement and arthroplasty is that a multitude of cements are available on the market. Although the durability of well-made cement mantles around implants is fairly consistent among cements, the products differ in terms of viscosity, working time, and setting. A surgeon must know the details of the particular cement he or she intends to use, as it will influence the cement technique. Working time and setting time vary among the different cements. Data have shown that different types of femoral stems should be inserted with different types of cements. For example, a rougher stem should be inserted in an earlier phase of cement polymerization, whereas a smoother stem should be inserted in a more doughy state. Therefore, a surgeon who uses a smooth stem should use cement with a longer doughy phase, whereas a surgeon who uses a rougher stem should use cement with a longer liquid phase. Failure to appreciate the working characteristics of the different cements can potentially lead to complications during the surgery.
The overall technique of cementing THR has evolved from first- to third-generation techniques (Table). Major improvements between these “generations” have been stratified in terms of bone preparation, cement preparation, and cement delivery. Improvements in bone preparation include the use of a plug for compression of cement, pulsatile lavage to remove loose cancellous bone, and blood to improve interdigitation of cement to bone and proximal pressurization of the cement mantle. Cement delivery has also been improved with the use of a cement gun to provide consistent retrograde filling of the canal followed by pressurization of the mantle. The literature supports improved outcomes in cemented THR with these improvements in cement techniques.
Cementing Technique
Bone preparation is critical for long-term survivorship of both the cemented stem and the cup.4 The aim is to provide a clean, stable bony bed for cement interdigitation into the remaining cancellous bone and to maintain stable interfaces between the implant and cement, and the cement and the bone.
Most investigators would agree that a surgeon should remove all loose cancellous bone but leave the remaining dense bone nearest to the cortex to enhance interdigitation of the cement into the remaining bone. This increases the shear strength of the cement and gives the best contact of the cement mantle to the remaining bone stock. Reaming with cylindrical or tapered reamers in the femur is often performed to remove the loosest bone but should be done by hand to leave a remnant of cancellous bone. It is important not to ream away all cancellous bone, as this will leave a smooth inner cortex and diminish the ability for the cement to bond to the bone. Some implant systems are designed to be reamer-less and all bone preparation is meant to be done by a broach. Broaching, which compacts the bone rather than removes it as a reamer does, is an important step in the femoral preparation. The broaches, which in many systems are also used for sizing and trialing of the femoral implant, create a reproducibly larger envelope of 2 mm to 3 mm circumferentially around the stem. This allows for a uniform thickness of the cement mantle around the stem. Aggressive broaching should be avoided to prevent denuding of the inner cortical bone.
Plugging the femoral canal improves the ability to pressurize the cement and limits the size and extent of the cement column. This increases the uniformity of the cement column. The canal can be occluded by bone, resorbable plugs, and, the most popular choice, polyethylene restrictors. Although a separate mixed batch of cement to plug the canal was shown by Harris to be the best occluder of the canal, it is a more time-consuming step and most surgeons today rely upon off-the-shelf polyethylene restrictors to plug the femoral canal. The more current restrictors are sized and have various fins and prominences, which enhance a surgeon’s ability to match the appropriate restrictor to the particular canal geometry. All of these plugs must be able to resist the forces generated by cement compression of 0.21-0.42 mPa.Ideally, the plug should be placed approximately 2 cm distal to the tip of the stem due to the high stresses seen at the stem tip but no further.6 There is no advantage to having the cement column extend any further beyond the stem, as this does not enhance fixation. Also, in the event of the need for cement removal for whatever reason, limiting the length of the cement column has many advantages.
| Generation
| Mixing/ Porosity Reduction
| Canal Preparation
| Insertion
| Centralization
|
| First |
Hand mix |
Rasp only, leave cancellous bone |
Manual insertion with finger packing |
None |
| Second |
Hand mix |
More aggressive rasp,
brushing pulsatile lavage |
Cement gun Distal canal plug
|
Early distal centralizers |
| Third |
Vacuum mix/ centrifugation
|
More aggressive rasp,
brushing pulsatile lavage |
Cement gun with
pressurization Distal canal plug |
Proximal and distal
centralizers
|
Once the bony bed has been broached, the cancellous bone compacted, and the canal plugged, the bone must be cleaned. Pulsatile lavage has been shown to be an effective means of removing further loose bone and fat content. This step has been shown to increase penetration of cement into the bone and has been considered critical in achieving an adequate cement interdigitation.4 Brushing the canal has not been shown to have any added value.
Once the bone has been cleaned, it should appear white, signifying that most blood and fat have been removed. Several authors believe that the bone should be dried to maintain this clean, white state. This can be achieved by using either hypotensive anesthesia or dilute epinephrine, or hydrogen peroxide mixtures. Frequent and regular drying of the canal with sponges will keep the field clean and dry. The drier the bone, the better the interdigitation and microlock of the cement to the bone.
Improvements in anesthetic techniques, such as hypotensive anesthetic techniques, have enhanced a surgeon’s ability to visualize the surgical field and to control blood loss. This improvement has been shown to keep the cleaned bony bed drier, which enhances the cement mantle considerably.
The cement can be mixed once the bone preparation has occurred. It has been shown that vacuum mixing and centrifugation can decrease cement porosity and fume exposure. Porosity reduction has been well documented to increase tensile and fatigue strength in the cement, theoretically increasing the cement’s longevity.7,8 The newer mixing systems are more user-friendly than the older mixing systems that were large and bulky.
Centralization has been shown to increase the likelihood of long-term success on the cemented femur. Both proximal and distal centralizers, which are now considered part of third-generation cement technique, are widely used as they have shown an increased ability to maintain a more uniform circumferential cement mantle around the stem.9 Consistently placing the stem in the center of the cement mantle has been shown to be a basic tenant of cement technique; centralizers are important in enabling the surgeon to reliably achieve this stem location.
Cement delivery has evolved. Although digital packing of the cement has been associated with a good deal of voids and cement mantle defects, the use of a caulking gun and the concept of retrograde filling of the canal have been instrumental in improving cement technique.10 A surgeon must ensure that the tip of the cement gun is placed at the tip of the plug so that the cement column begins directly on the tip of the plug and then, with steady pressure on the handle, a surgeon should allow the cement column itself to gently force the gun’s syringe back out of the bone. It is important to avoid the common mistake of having the cement migrate proximally while it is being introduced around the syringe. Removing the syringe from this type of a cement column leaves a defect in the mantle.
The timing of cement introduction depends upon the type of cement being used. The doughier (fast setting) cements must be introduced right away and sometimes cannot be used with a gun because of the resistance generated by the cement. The lower viscosity cements must be placed later in their setting cycle to avoid the cement running out of the canal and leaving retained cement around the joint. The ideal time for cement introduction is when the cement is just becoming doughy with a dull appearance and not sticky. The cement guns consistently deliver cement at pressures that can decrease the chances of blood mixing with the cement at the bone-cement interfaces and have been shown to decrease the incidence of air voids.
Once the cement column has been applied, it should be pressurized to further increase interdigitation and microlock. This can be accomplished by placing the thumb over the top of the canal and manually pressurizing the cement or by applying a cone or disk to the cement gun to improve proximal pressurization. This method has been shown to generate pressures >30 mm Hg in the proximal cement mantle.11
When the cement has been pressurized, the stem is ready to be inserted. It is essential that the stem be inserted accurately into the envelope, which had been created by the broach. Cement mantle thickness is important. Although the ideal thickness is the subject of debate, it has been shown that stems with a 2-mm to 5-mm medial mantle had the best outcome12 and that 3-mm to 4-mm cement mantles appear to have the best stress curves.13 The stem should be centrally aligned in the canal.
A stem introducer, which can control the version of the stem while it is being introduced, is a helpful tool. The optimal time for stem insertion is when the cement is in a slightly doughy shape as this has been associated with the best cement penetration. Gentle steady manual pressure should be applied with version controlled by an inserter. It is imperative to hold both the leg and implant in place while the cement cures to avoid the creation of cement voids. All excess cement can be removed at this time.
Acetabulum
On the acetabular side, the concepts are similar to the femur; removal of loose cancellous bone, cleaning of bony surfaces, and pressurization of cement into the bony bed. The bone should be reamed until cancellous bone is visualized and special attention should be paid to bone preparation and pressurization in zone 1.14,15 All pelvic cysts should be curetted, cleaned, and grafted. Anchor holes should be placed into the bone to improve long-term fixation.
The bone should be dried. However, drying the bone is difficult to achieve on the acetabulum, as there is no canal to plug to limit bleeding. Sponges with a low concentration of thrombin have been used in the past.
The surgeon should use the hand or a gun to place cement in a doughy state into the acetabulum. Although the acetabulum can be difficult to pressurize, it should be pressurized as best as possible. A few pressurizers are commercially available, but using a surgical glove placed over a slightly under-sized reamer is often sufficient. An introducer for the all-polyethylene cup is helpful to maintain accurate orientation of the implant in the cement mantle while the cement cures. It is imperative that a surgeon assesses appropriate version and abduction because, once the cement has cured, it is not possible to move the cup. Extruded cement must be removed carefully to prevent impingement and/or third-body wear.
With the current interest in smaller incisions, adequate visualization sometimes can be difficult. It is important not to compromise the visibility of the pelvis at this stage, which may cause malorientation of the now immovable cup or cause a surgeon to miss retained cement after it has cured.
Many factors influence the overall survivorship of a THR including patient selection, implant choice, and design, but progress has been made in the technique of cementing THR. These contemporary cement techniques include appropriate cement choice, careful bone preparation (broaching and cleaning), canal occlusion, appropriate cement preparation to limit voids, retrograde filling, cement pressurization, and the use of centralizers.





