


Bile duct cancer (Cholangiocarcinoma) treatment and surgery India offers information on Bile duct cancer (Cholangiocarcinoma) Doctor India, Bile duct cancer (Cholangiocarcinoma) treatment and surgery Hospital India, Bile duct cancer (Cholangiocarcinoma) treatment and surgery Abroad, Bile duct cancer (Cholangiocarcinoma) causes, symptoms, Risk factors, treatment and surgery.
Bile duct cancer
Causes and risk factors
Signs and symptoms
How it is diagnosed
Laparotomy
Staging and grading
Treatment overview
Surgery
Stent insertion
Other treatments
Clinical trials
Your feelings
References
Bile duct cancer
The bile ducts are the tubes connecting the liver and gall bladder to the small intestine (small bowel). Bile is a fluid made by the liver and stored in the gall bladder. Its main function is to break down fats during their digestion in the small bowel. In people who have had their gall bladder removed, bile flows directly into the small intestine. The bile ducts and gall bladder are known as the biliary system.
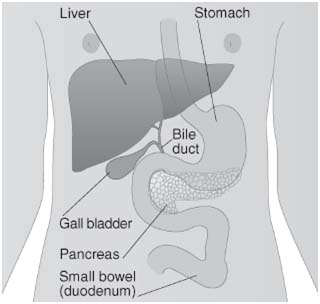
Cancer is classified according to the type of cell from which it starts. Cancer of the biliary system almost always starts in a type of tissue called glandular tissue and is then known as adenocarcinoma.
If the cancer starts in the part of the bile ducts contained within the liver it is known as intra-hepatic. If it starts in the area of the bile ducts outside the liver it is known as extra-hepatic. This information concentrates mainly on extra-hepatic bile duct cancers. Intra-hepatic bile duct cancers may be treated like primary liver cancer.
Causes and risk factors
The cause of most bile duct cancers is unknown. There are a number of risk factors that can increase your risk of developing bile duct cancer.
These are:
Inflammatory bowel disease People who have a chronic inflammatory bowel condition, known as ulcerative colitis, are at an increased risk of developing this type of cancer.
Abnormal bile ducts People who are born with (congenital) abnormalities of the bile ducts, such as choledochal cysts, are more at risk of developing cholangiocarcinoma
Infection In Africa and Asia, infection with a parasite known as the liver fluke is thought to cause a large number of bile duct cancers.
Bile duct cancer, like other cancers, is not infectious and cannot be passed on to other people.
Signs and symptoms
If cancer develops in the bile ducts it may block the flow of bile from the liver to the intestine. This causes the bile to flow back into the blood and body tissues, and leads to the skin and whites of the eyes becoming yellow (known as jaundice). The urine also becomes a dark yellow colour and stools (bowel motions) are pale. The skin may become itchy. Mild discomfort in the abdomen, loss of appetite, high temperatures (fevers) and weight loss may also occur.
These symptoms can be caused by many things other than bile duct cancer, but any jaundice or any symptoms which get worse or last for a few weeks should always be checked by your doctor.
How it is diagnosed
Usually you begin by seeing your GP, who will examine you. They will refer you to a hospital specialist for any tests that may be necessary and for expert advice and treatment.
At the hospital the doctor will ask you about your general health and any previous medical problems. They will also examine you and take blood samples to check your general health and that your liver is working properly.
The following tests are commonly used to diagnose bile duct cancer :
Ultrasound scan : Sound waves are used to make up a picture of the bile ducts and surrounding organs. These scans are done in the hospital's scanning department. You will be asked not to eat, and to drink clear fluids only (nothing fizzy or milky) for four to six hours before the scan. Once you are lying comfortably on your back, a gel is spread onto your abdomen. A small device, like a microphone, is then rubbed over the area. The sound waves are converted into a picture using a computer. The test is completely painless and takes 15–20 minutes.
CT (computerised tomography) scan : A CT scan takes a series of x-rays which are fed into a computer to build up a detailed picture of your bile ducts and surrounding organs. On the day of the scan you will be asked not to eat or drink anything for at least four hours before your appointment. You will be given a special liquid to drink an hour before the test and again immediately before the scan. The liquid shows up on x-ray to ensure that a clear picture is obtained.
Once you are comfortably positioned on your back on the couch, the scan can be taken. About half-way through the scan a special dye will be injected into the vein to show up the blood vessels. This may make you feel warm or 'flushed' for up to half an hour. The test itself is completely painless, but it will mean that you have to lie still for about 10–30 minutes. If you had little to drink before the scan, you may be advised to drink plenty afterwards to make up for this.
MRI (magnetic resonance imaging) scan : This test is similar to a CT scan, but uses magnetism instead of x-rays to build up cross-sectional pictures of your body. During the test you will be asked to lie very still on a couch inside a large metal cylinder which is open at both ends. The whole test may take up to an hour. It can be slightly uncomfortable and some people feel a bit claustrophobic during the scan, which is also very noisy. You will be given earplugs or headphones to wear. A two-way intercom enables you to talk with the people controlling the scanner.
ERCP (endoscopic retrograde cholangiopancreatography) : This is a procedure by which an x-ray picture of the pancreatic duct and of the bile duct can be taken. It may also be used to unblock the bile duct if necessary.
You will be asked not to eat or drink anything for about six hours before the test so that the stomach and duodenum (first part of the small bowel) are empty. You will be given an injection to make you relax (a sedative) and a local anaesthetic spray will be used to numb your throat. The doctor will then pass a thin flexible tube known as an endoscope through your mouth into your stomach and into the duodenum just beyond it. Looking down the endoscope, the doctor can find the opening through which the bile duct and the duct of the pancreas drain into the duodenum. A dye which can be seen on x-ray can be injected into these ducts and the doctor will be able to see whether there is any abnormality or any blockage in the ducts.
If there is a blockage it may be possible or the doctor to insert a small tube known as stent. You may have some discomfort during this procedure; if you do, it is important that you let your doctor know. You will be given antibiotics beforehand (to help prevent any infection) and will probably stay in hospital for one night afterwards.
PTC (percutaneous transhepatic cholangiography) : This is another procedure by which your doctor can obtain an x-ray picture of the bile duct. You will be asked not to eat or drink anything for about six hours before the test and will be given a sedative as for the ECRP.
An area on the right side of your abdomen will be numbed with a local anaesthetic (an injection) and a thin needle will be passed into the liver through the skin. A dye will be injected through the needle into the bile duct within the liver. X-rays will then be taken to see if there is any abnormality or blockage of the duct.
You may feel some discomfort as the needle enters the liver. You will be given antibiotics before and after this procedure (to help prevent infection) and you will stay in hospital for at least one night afterwards.
Angiography : As the bile duct is very close to the major blood vessels of the liver, a test called an angiogram may be done. The angiogram can check whether the blood vessels are affected by the tumour.
A fine tube is inserted into an artery in your groin and a dye is injected through the tube. The dye circulates in the arteries to make them show up on x-ray. An angiogram is carried out in a room within the x-ray department. Sometimes an MRI scan can be used to show up the blood vessels of the liver and then an angiogram will not be necessary.
Biopsy : The results of the previous tests may make your doctor strongly suspect a diagnosis of cancer of the bile duct, but the only way to be sure of the diagnosis is to take some cells or a small piece of tissue from the affected area of the bile duct to look at under a microscope. This is called a biopsy and may be carried out during an ECRP or PTC.
A fine needle is passed into the tumour through the skin after the area has been numbed using a local anaesthetic injection. CT or ultrasound may be used at the same time, to make sure that the biopsy is taken from the right place.
Endoscopic ultrasound scan (EUS) : This scan is similar to an ERCP but involves an ultrasound probe being passed down the endoscope to take an ultrasound scan of the pancreas and surrounding structures.
Laparotomy
If the doctor cannot make the diagnosis from the above tests, a procedure called a laparotomy may be done under a general anaesthetic. This involves making a cut (incision) into your abdomen so that the surgeon can examine the bile duct and the tissue around it for cancer. Sometimes this examination can be done through a tiny cut using a camera called a laparoscope – this procedure is known as keyhole surgery.
If a cancer is found, but looks as though it has not spread to surrounding tissues, the surgeon may be able to remove the cancer or relieve any blockage that it is causing.
Staging and grading
Staging
The stage of a cancer is a term used to describe its size and whether it has spread beyond its original site. Knowing the particular type and the stage of the cancer helps the doctors to decide on the most appropriate treatment.
Cancer can spread in the body, either in the blood stream or through the lymphatic system. The lymphatic system is part of the body’s defence against infection and disease. The system is made up of a network of lymph glands (also known as lymph nodes) that are linked by fine ducts containing lymph fluid. Your doctors will usually look at the lymph nodes close to the biliary system in order to find the stage of your cancer.
The cancer is contained within the bile duct.
The cancer has spread through the wall of the bile duct but has not spread into nearby lymph nodes or other structures.
The cancer has spread into the liver, pancreas or gall bladder or to the nearby blood vessels, but not the lymph nodes.
The cancer has spread into nearby lymph nodes.
The cancer is affecting the main blood vessels that take blood to and from the liver, or it has spread into the small or large bowel, the stomach or the abdominal wall. Lymph nodes in the abdomen may also be affected.
The cancer has spread to distant parts of the body such as the lungs.
If the cancer comes back after initial treatment, this is known as recurrent cancer.
Grading
Grading refers to the appearance of the cancer cells under the microscope and gives an idea of how quickly the cancer may develop. Low-grade means that the cancer cells look very like normal cells; they are usually slow-growing and are less likely to spread. In high-grade tumours the cells look very abnormal, are likely to grow more quickly and are more likely to spread.
Treatment overview
The type of treatment that you are given will depend on a number of factors, including your general health, the position and size of the cancer in the bile duct and whether the cancer has spread beyond the bile duct.
Consent
Before you have any treatment, your doctor will give you full information about what it involves and explain the aims of the treatment to you. They will usually ask you to sign a form saying that you give permission (consent) for the hospital staff to give you the treatment. No medical treatment can be given without your consent.
Benefits and disadvantages of treatment
Treatment can be given for different reasons and the potential benefits will vary for each person. If you have been offered treatment that aims to cure your cancer, deciding whether to have the treatment may not be difficult. However, if a cure is not possible and the treatment is to control the cancer for a period of time, it may be more difficult to decide whether or not to go ahead.
If you feel that you can't make a decision about treatment when it is first explained to you, you can always ask for more time to decide.
You are free to choose not to have the treatment and the staff can explain what may happen if you don't have it. You don't have to give a reason for not wanting to have treatment, but it can be helpful to let the staff know your concerns so that they can give you the best advice.
Surgery
Surgery may be used to remove the cancer if it has not spread beyond the bile duct. It is not always possible to carry out surgery, as the bile duct is in a difficult position and it may be impossible to remove the cancer completely. The decision about whether surgery is possible or not depends on the results of the tests described above. If surgery is recommended then you will be referred to a surgeon with a special interest in this rare cancer.
There are different operations depending upon how big the cancer is and whether it has begun to spread into nearby tissues.
Removal of the bile ducts If the cancer is small and contained within the ducts, then just the bile ducts containing the cancer are removed and the remaining ducts in the liver are joined to the small bowel, allowing the bile to flow again.
Partial liver resection If the cancer has begun to spread into the liver, the affected part of the liver is removed, along with the bile ducts.
Whipple's If the cancer is larger and has spread into nearby structures, then the bile ducts, part of the stomach, part of the duodenum (small bowel), the pancreas, gall bladder and the surrounding lymph nodes are all removed.
After your operation you may stay in an intensive-care ward for the first couple of days. You will then be moved to a general ward until you recover. Most people need to be in hospital for up to two weeks after this type of operation.
Bypass surgery Sometimes it isn't possible to remove the tumour and other procedures may be performed to relieve the blockage (obstruction) and allow the bile to go into the intestine. The jaundice will then clear up.
The surgical method of dealing with blockage of the bile duct involves joining the gall bladder (or the bile duct) to part of your small bowel. This bypasses the blocked part of the bile duct and allows the bile to flow from the liver into the intestine. This operation is called a cholecysto-jejunostomy or cholecysto-duodenostomy if the gall bladder is used. It is called a hepatico-jejunostomy if the bile duct is used.
Another type of operation may be necessary if the duodenum is also blocked. This is called a gastrojejunostomy and involves connecting a piece of the small bowel (the jejunum) to the stomach to bypass the duodenum. This will stop the persistent vomiting (being sick) that can occasionally happen if the cancer blocks the duodenum.
Stent insertion
There are two ways in which it may be possible to relieve jaundice without a surgical operation. These use the ERCP or PTC procedures described below.
The ERCP method involves the insertion of a tube, called a stent into the blocked bile duct. The stent is about as thick as a ball-point pen refill and about 5–10cm long (two to four inches). The stent clears a passage through the bile duct to allow the bile to drain away. The preparation and procedure is the same as for ERCP described above. By looking at the x-ray image the doctor will be able to see the narrowing in the bile duct. The narrowing can be stretched using dilators (small inflatable balloons), and the stent can then be inserted through the endoscope to enable the bile to drain.
The tube usually needs to be replaced every three to four months to prevent it becoming blocked. If the tube does block, recurrent high temperatures and/or return of the jaundice will occur. It is important to tell your specialist about these symptoms as early as possible. Antibiotic treatment may be needed and your specialist may advise that the stent is exchanged for a new one. This procedure can be done relatively easily for most people.
During the PTC method, the procedure and the preparation you will need is as described in the section about PTC. A temporary wire is passed to the area of blockage and the stent is guided along the wire. Sometimes a drainage tube (catheter) is left in the bile duct. One end of the catheter is in the bile duct and the other lies outside the body connected to a bag, which collects the bile. This is to help with the insertion of the stent or, sometimes, to enable x-rays to be taken to check the position of the stent after it has been put in place. It is usually left in for a few days. Once the catheter is removed the hole heals over within two days. You will be given antibiotics before and after the procedure to help prevent any infection. It is likely that you will stay in hospital for a few days.
Sometimes, if the bile duct cannot be opened easily from the small intestine during ERCP, a combination of ERCP and PTC may be used.
Other treatments
Radiotherapy
Radiotherapy is occasionally used to treat bile duct cancer. Radiotherapy treats cancer by using high-energy x-rays to destroy cancer cells while doing as little harm as possible to normal cells. It may be given either externally from a radiotherapy machine, or internally by placing radioactive material close to the tumour.
Chemotherapy
Chemotherapy is the use of anti-cancer (cytotoxic) drugs to destroy the cancer cells. They work by disrupting the growth of cancer cells. Occasionally, chemotherapy may be given in combination with radiotherapy for cancers that cannot be removed surgically. Researchers are still looking into how effective chemotherapy is for the treatment of bile duct cancer.
Photodynamic therapy (PDT)
PDT uses a combination of laser light of a specific wavelength and a light-sensitive drug to destroy cancer cells. In bile duct cancer it is used to help relieve symptoms.
The light-sensitive drug (a photosensitising agent) is injected into a vein. It circulates in the bloodstream and enters cells throughout the body. The drug enters more cancer cells than healthy cells. It does not do anything until it is exposed to laser light of a particular wavelength. When a laser is shone on to the cancer, the drug becomes active and destroys the cancer cells.
Clinical trials
Research into treatments for bile duct cancer is ongoing and advances are being made. Cancer doctors use clinical trials to assess new treatments.
You may be asked to take part in a clinical trial. Your doctor must discuss the treatment with you so that you have a full understanding of the trial and what it means to take part.
Clinical trials
Research into treatments for bile duct cancer is ongoing and advances are being made. Cancer doctors use clinical trials to assess new treatments.
You may be asked to take part in a clinical trial. Your doctor must discuss the treatment with you so that you have a full understanding of the trial and what it means to take part.
Bile Duct Cancer Treatment India,Bile Duct Diagnosis,Bile Duct Cancer, Bile Duct Cancer Treatment, India Surgery Bile Duct Diagnosis, India Surgery Treatment, India Surgery Bile Duct, India Surgery Bile Duct Cancer, India Surgery Bile Duct Cancer Diagnosis, India Surgery Tour, India Surgery Cholangiocarcinoma, India Surgery Whipple Surgery, India Surgery Laparoscopic Cholecystectomy, India Surgery Gallbladder, India Surgery Primary Cancers, India Surgery Symptoms Of Bile Duct Cancer, India Surgery Extrahepatic, India Surgery Bile Duct Cancer Treatment Hospitals, India Surgery Tour, India Surgery Chemotherapy, Ndia Surgery Cancer Of The Bile Ducts, India Surgery Radiotherapy, India Surgery Supportive, India Surgery Support, India Surgery Care, India Surgery Cancer Treatment