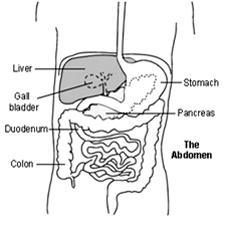
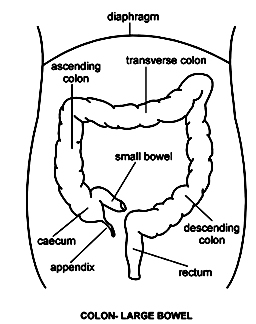
India Surgery Sigmoid Colectomy,Cost Laparoscopic Sigmoid Colectomy, Sigmoid Colectomy Surgery, Surgical Operations, India Laparoscopic Sigmoid Colectomy, India Sigmoid Colectomy Surgery, India Sigmoid Colectomy Surgical Operations, India Surgery Tour, India Best Sigmoid Colectomy Surgery, India Sigmoid Colectomy Surgery Hospital, India Left Side Of The Colon, India Low Cost Sigmoid Colectomy, India Remove Left Side Of The Colon, India Cancer, India Surgery India Sigmoid-Colectomy, India Best Surgery India Sigmoid Colectomy, India Sigmoid Colectomy Surgery Clinic, India Sigmoid-Colectomy Surgery Hospital Delhi